Your cart is currently empty!
Common Overlooked Points That a PALS Pretest Teaches You
Pediatric patients represent a major concern for health professionals, and unfortunately, up to 16,000 children suffer cardiac arrest each year, reports the American Association of Nurse Anesthetists (AANA). In addition, one in 10,000 children suffer an out-of-hospital (OOH) respiratory arrest, such as that caused by unintentional drowning, reports the National Library of Medicine. Sudden cardiac or respiratory arrest in children occurs less often than adults, and the exceptions often involve congenital health problems.
Pediatric Advanced Life Support (PALS) provides the step-by-step recommendations for treating children in arrest or that begin to exhibit symptoms of an impending arrest, such as labored breathing. Clearly, recognizing these indicators amounts to saving lives, and a PALS pretest, such as the test here, can help health professionals achieve this feat. In addition, care providers must understand the most overlooked areas of PALS, especially when symptoms may cause confusion between the proper steps to take for a child versus an adult. Completing a PALS pretest helps to tackle these overlooked areas when providing life-saving care, such as the skills gained in an online course, located here, to pediatric patients.
Recognizing When to Begin Life-Saving Measures Despite Presence of a Pulse
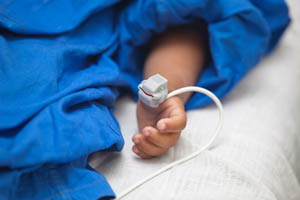 Before even considering whether a child needs life-saving care, it is important to understand when the presence of a pulse can require initiation of the PALS algorithm. As noted in a past blog here, assessing a child in distress includes feeling for the presence of pulse and determining whether the heart rate requires chest compressions. For example, one arrhythmia, Bradycardia, which refers to a decreased heart rate, may result in a pulse of less than 60 beats per minute (BPM). Any pulse below 60 BPM warrants the initiation of chest compressions to prevent cardiac arrest. Depending on the possible causes of arrest and other symptoms, such as labored breathing, initiations of the PALS algorithm may be necessary.
Before even considering whether a child needs life-saving care, it is important to understand when the presence of a pulse can require initiation of the PALS algorithm. As noted in a past blog here, assessing a child in distress includes feeling for the presence of pulse and determining whether the heart rate requires chest compressions. For example, one arrhythmia, Bradycardia, which refers to a decreased heart rate, may result in a pulse of less than 60 beats per minute (BPM). Any pulse below 60 BPM warrants the initiation of chest compressions to prevent cardiac arrest. Depending on the possible causes of arrest and other symptoms, such as labored breathing, initiations of the PALS algorithm may be necessary.
Furthermore, heart rates are typically faster in younger children, notes Pediatrics for Medical Students, so even rates in the 70-80 range may be insufficient for ensuring oxygen perfusion. Poor perfusion leads to a hypoxic state in tissues, which may result in tissue damage and even death. Recognizing typical vital signs for a child of different age groups may be included on a PALS pretest.
Incorrectly Assessing a Patient With the Glasgow Coma Scale
The Glasgow Coma Scale (GCS) uses indicators of consciousness to assess a child’s state of mind. These are typically responses that can be seen with the naked eye, so it is possible for the PALS pretest to review the key factor in providing PALS, such as maintaining blood volume to prevent shock, and whether such actions would be part of as assessment on the GCS.
Inaccurate Recognition or Charting of Breathing Sounds
A PALS pretest tackles the assessment issue further by considering the terminology used to describe a patient’s symptoms. More importantly, the right terminology is crucial to ensuring all members of the care team understand the child’s symptoms and how to best treat them. For instance, absent and decreased sounds may result from air or fluid within the chest wall, reports Medline Plus. Meanwhile, the most common abnormal breath sounds include:
- Rales – The lungs make these sounds when a person inhales, and they include a small clicking, rattling or bubbly noise in the chest. The sounds can also be described further as fine, coarse, dry or moist. For instance, small, clear clicking sounds would be dry. Moist would apply to bubbling sounds. Coarse sounds may remind a person of rubbing against a brick wall, and fine sandpaper on wood mirrors a “fine” sound. The key to distinguishing rales lies in their short-lived noise.
- Wheezing – This is among the most recognizable lung sounds. Wheezing occurs when the airways narrow and cause a high-pitched sound to escape.
- Rhonchi – Rhonchi may sound like snoring, and they exist when the airway is blocked or becomes overly rough.
- Stridor – This sound closely resembles wheezing, but it not necessarily wheezing as the sound comes from an area closer to the mouth. Typically, stridor is caused by a blocked airway in the trachea or the back of the throat, such as following a choking incident or anaphylactic reaction.
Making Hasty Decisions That Increase Risk When Other Options Exist
Completing a PALS pretest puts pressure on a person to assess the best option for treating children in respiratory or cardiac arrest. However, the questions will not necessarily reflect all accurate options. In other words, some may ask for the best solution to a problem, such as an obstructed airway. The test also checks your consideration of other factors, such as risk for complications and unnecessary injury.
For example, a patient appearing in distress may be a candidate for an intraosseous catheter, but that option lacks value and rationale if an intravenous access can be established to provide the same effect. At the same time, the care provider must consider the needs of the patient and how to respond in an emergency. All decisions must be made immediately, but they must follow a structure, identifying the issue, the best treatment measure, the likely cause, how to treat that cause and how to prevent its recurrence.
The list of hasty, poorly planned decisions is endless, so it is best to approach PALS from a limited care standpoint. The simplest solution to correct the problem and to avoid unnecessary treatment is often the best. This is a key reason those working in pediatric facilities should take a PALS pretest and ensure their skills reflect the latest standards for treatment.
Medication Administration Errors in Treating Certain Problems
 As explained in past article, available here, medications used in the administration of life-saving measures are continuously under review by the International Liaison Committee on Resuscitation (ILCOR). In recent years, the administration of medications to correct arrhythmias, also known as antiarrhythmic drugs, and even epinephrine has come under the scope of the review. Recommendations change to reflect the latest data and studies to increase the chances of survival. A PALS pretest will provide an opportunity to test your knowledge of the most updated changes to medication administration.
As explained in past article, available here, medications used in the administration of life-saving measures are continuously under review by the International Liaison Committee on Resuscitation (ILCOR). In recent years, the administration of medications to correct arrhythmias, also known as antiarrhythmic drugs, and even epinephrine has come under the scope of the review. Recommendations change to reflect the latest data and studies to increase the chances of survival. A PALS pretest will provide an opportunity to test your knowledge of the most updated changes to medication administration.
Furthermore, ILCOR emphasizes studies conducted on the use of antiarrhythmic drugs took place during the initial years after the ILCOR recommendations for minimal interruptions in chest compressions were introduced. As a result, the information gained through more data on the use of amiodarone and lidocaine for arrhythmias cannot necessarily be considered with its impact the arrhythmia alone. Any assessment must consider the impact of other improvements, including high-quality, uninterrupted compressions. So, the only solution to the problem lies in both continuing high-quality, uninterrupted compressions and administering medications as indicated by the most recent guidelines, even when such guidelines would have replaced existing recommendations.
Distractions Within the Room That Result in Mistakes
Distractions within the exam room make for another opportunity to overlook PALS guidelines. Parents, family members, and other members of the care team all want to know what is happening, what can be fixed, and what the outcome will be? Unfortunately, this combination adds to the risk of missed symptoms and failure to identify the cause of distress. Such issues may result in an inaccurate assessment of breathing sounds, which may result in a misdiagnosis.
For example, if the commotion in the room obscures the sounds of stridor, the care team may assume pneumonia is the culprit. In reality, the patient may have choked on something, blocking off the upper airway. Moreover, distractions can make it difficult to notice sites of increased respiratory distress, such as head bobbing or nasal flaring. A PALS precourse self-assessment will review these symptoms and their impact on decisions as part of the PALS algorithm. Those that miss more than one question should consider reviewing the symptoms of respiratory or cardiac distress.
Poor Communication Among Parents, Children and Health Professionals
Communication plays a vital role in reducing the risk of subsequent cardiac arrest or initial cardiac arrest for children experiencing major health problems. Health care professionals must clearly communicate with one another when providing PALS, and they must obtain information from parents and children as well. Since the basis for PALS goes back to treating the reversible causes of arrest or distress, a deliberate communication process must be included within the PALS protocols, reports NCBI.NLM.HIH.Gov.
In other words, health care professionals should know how to communicate with children to know what hurts, listen and look for signs of distress that a child may indicate through body language and work together with parents or caregivers to understand the events leading up to the onset of the illness. The same practice applies to learning from each experience in providing PALS as a care team. The PALS pretest contains subtle indicators that allude to the need for collaboration and communication, including working together to restore patency in a child or treating shock.
Lack of Practice Resulting in Confusion Between Adult and Pediatric Algorithms
A final area of concern goes back to misconceptions about actions for pediatric patients compared to adults. This is like the need to recognize low heart rates as a cause to start chest compressions. However, it carries added weight for ensuring medications are tailored to the specific weight of the child. Even oxygen saturation becomes an issue in this instance.
Generally, oxygen saturation above 92% may be considered sufficient. Yet, that is only true for adults. A child’s oxygen saturation must be higher to account for the increased rate of metabolism. The PALS pretest will review oxygen saturation minimums, and it may also review the practices useful to increase saturation, such as increased supplemental oxygen flow rate or even the use of an oxygen mask.
Know the Most Overlooked Aspects of PALS; Pinpoint Weaknesses in Your Skills With a PALS Pretest Too
The Centers for Disease Control and Prevention (CDC) published the most recent Childhood Injury Report in 2008. The report revealed more than 12,000 children lose their lives each year after an unintentional injury. Unfortunately, the age of that report means actual mortality statistics have increased in accordance with population growth. Regardless of statistics, all pediatric patients deserve every chance at life, and health professionals stand in the positions to help children overcome illnesses that could cost their lives.
The time to review your PALS skills is not when a child lies on a bed unable to get enough oxygen; the time to review is well before a child every enters the hospital or care center. Health professionals must recognize the signs of distress, especially in children unable to voice their problems, such as infants and those with intellectual or developmental disabilities. Taking a PALS pretest can help health professionals review their skills and learn more about the most overlooked aspects of PALS. The nature of PALS brings cardiac problems to mind, but it is more expansive. In addition, pediatric vital signs and symptoms may still require immediate intervention even when those symptoms would appear meaningless in adults, such as those with an oxygen saturation below 95% or with a pulse of less than 60 bpm. You can overcome the weaknesses in your skills, provided you know what they are.
Have you ever forgotten or overlooked a key component of PALS when treating a child in need? If so, share your experiences along with this article to your social media accounts. Everyone makes mistakes, but mistakes in providing care can cost lives. Also, remember to take your PALS pretest, which is available here, and consider reviewing your skills in their entirety as well.









Leave a Reply