Your cart is currently empty!
Content Updates Based on the Latest ILCOR Guidelines
2020-2025 ILCOR Guideline Updates
While the ILCOR releases its updated guidelines and recommendations in 5-year cycles, with the last round of updates being the 2020-2025 guidelines, researchers have committed to a continuous evidence-evaluation process. These research-driven updates have allowed us to update our material as new recommendations emerge, ensuring our lifesavers are equipped with the most current life-saving information. We have made many critical updates to our content in the last year based on these recommendations.
Changes in CPR
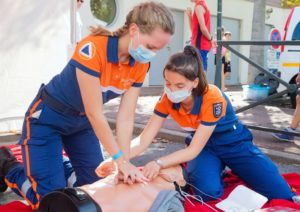 The newest ILCOR guidelines have reiterated the importance of early intervention in CPR. Delivering compressions and breaths early helps to reduce the depletion of oxygen and improves blood flow, which is essential for preventing cardiac arrest. We have adapted our content to highlight the importance of bystander intervention in these scenarios.
The newest ILCOR guidelines have reiterated the importance of early intervention in CPR. Delivering compressions and breaths early helps to reduce the depletion of oxygen and improves blood flow, which is essential for preventing cardiac arrest. We have adapted our content to highlight the importance of bystander intervention in these scenarios.
Immediately after calling for help, rescuers should begin CPR. Once rescuers can call for help, they should use a speaker phone for a hands-free phone call option. Our content now emphasizes special instructions for scene safety and guidance on what to do in an emergency when waiting for a medical professional or team to arrive.
In addition to layperson intervention, the latest guidelines also differentiate between child and infant CPR recommendations depending on if the CPR is done by a single rescuer or a team of two or more rescuers.
Child/Infant CPR Updates and Their Effects on PALS and BLS
With the new distinctions between one-rescuer and two-rescuer interventions, our Pediatric Advanced Life Support (PALS) content and Basic Life Support (BLS) content have also been affected. We have updated the guidelines throughout this content to reflect the main changes in CPR, airway management, and delivery of rescue breaths. Below are the current recommendations we are following for single rescuers and teams of two or more rescuers delivering CPR.
One Rescuer Recommendation:
- Before getting additional help, one rescuer should quickly perform 5 sets of CPR
- One set of CPR consists of 30 compressions and two breaths
Two Rescuer Recommendation:
- Before getting additional help, teams of two rescuers should quickly perform 10 sets of CPR
- One set of CPR consists of 15 compressions and two breaths
For airway management in children or infants experiencing cardiac arrest, the guidelines listed below are based on the latest ILCOR suggestions and vary depending on the number of rescuers present. The updated compression-to-breath ratios also differ depending on whether or not an advanced airway is in place.
One Rescuer Recommendation for Advanced Airway:
- One breath every 6 seconds without pauses in compressions
- 10-15 breaths per minute
Two Rescuer Recommendation for Advanced Airway:
- One breath every 2-3 seconds without pauses in compressions
- 20-30 breaths per minute
One Rescuer Recommendation for NO Advanced Airway:
- 30 compressions followed by 2 breaths
Two Rescuer Recommendation for NO Advanced Airway:
- 15 compressions followed by 2 breaths
Note we have also updated airway management for adults. If an advanced airway is present, one breath every 6 seconds without pauses in compressions should be delivered in an adult.
For a more comprehensive overview of pediatric guidelines affected by the most recent ILCOR recommendations, consider enrolling in a Pediatric Advanced Life Support course.
CPR Administration Updates
It is now recommended to start CPR with compressions rather than ventilation. The recommended CPR procedure can be remembered as C-A-B or compressions-airway-breaths.
CPR should be administered on a firm surface when possible. The ILCOR task force emphasizes that effective compressions can still be achieved on a soft surface if the provider compensates by increasing compression depth. Still, the latest guidelines have been updated to recommend moving a patient from a bed to the floor, when possible, to achieve a firmer surface.
No matter your medical background or experience, everyone has the ability to learn CPR and save a life. To learn more about CPR and how to prepare yourself for a life-threatening situation, enroll in a CPR, AED, and First Aid course today.
We have made these changes to our English CPR and BLS courses and content, but we have also updated our Spanish CPR and BLS content to reflect these updates.
ACLS 2020-2025 Updates
Based on the emphasized importance of working in teams, we have added a section highlighting successful team dynamics of the resuscitation team in Advanced Cardiac Life Support (ACLS). The resuscitation team continues to be recognized as a key role in advanced life support, and good team dynamics aid in the success of these teams.
Introduction to Targeted Temperature Management (TTM)
We have updated our sections that were previously based on therapeutic hypothermia to be inclusive of all targeted temperature management (TTM). Our updated section provides guidance for achieving and maintaining a specific body temperature in an affected individual.
Common Drug Administration in ACLS
When blood pressure is extremely low and the individual is not in cardiac arrest, the pressors of choice are dopamine and norepinephrine. Vasopressin and Phenylephrine are the second agents to be added, and epinephrine is generally only reserved for severe hypotension or as a last-line agent. Epinephrine remains the suggested vasopressor to be administered during cardiac arrest.
In terms of routes for drug delivery for adults in cardiac arrest, the ILCOR now recommends the intravenous (IV) route be used for the first attempt. If IV attempts fail or IV access is not feasible, the Intraosseous (IO) route is suggested. Long-term effects of drug delivery by IV or IO route are still being studied, but the IV route is currently favored amongst ILCOR researchers within the Advanced Life Support (ALS) Task Force. To stay up-to-date on these findings, it is recommended to recertify in ACLS at least once every two years.
Our newest content also reflects the updated doses of common drugs. When treating symptomatic bradycardia, we now recommend a 1mg dose of Atropine every three minutes, as opposed to a .5mg dose. We still recommend a maximum dose of 20mg when administering Dopamine but have updated the range to a 5-20mcg/kg/min dose for Shock/CHF and symptomatic bradycardia treatment.
Newest Additions to ACLS
Our first addition to our Advanced Cardiac Life Support content is the FAST acronym, an acronym based on the Cincinnati Pre-Hospital Stroke Scale. The acronym is designed to evaluate if and when an individual is having a stroke. Through the acronym, we advise monitoring an individual’s Face, Arms and Speech and the expected amount of Time to assess the individual and call emergency services.
The recovery process after suffering a cardiac arrest can be extensive and should continue long after initial hospitalization. We have updated our content to reflect the necessary formal assessment and continued support following a cardiac arrest. A new checklist we have designed for post-cardiac arrest care can be remembered as “VOMIT.” This acronym includes five specific things to check for in post-cardiac arrest patients, including: Vital signs, Oxygen, Myocardial infarction, IV, and Targeted Temperature Management.
Our largest update has been the implementation of an entirely new ACLS Rhythms and Interpretation section. This section overviews common categories of ACLS rhythms and identifies the most common ACLS rhythms.
The Latest Updates to Basic Life Support and First Aid
Foreign Body Airway Obstruction (FBAO)
Foreign Body Airway Obstruction (FBAO), commonly understood as “choking,” is currently the fourth leading cause of unintentional death in the United States. Due to the severity of FBAO, if unrelieved, this topic is constantly under review. In their most recent publications, the ILCOR task force has updated their suggestions for relieving FBAO.
To relieve FBAO in conscious adults and children over the age of one, you should first use back slaps and then move to abdominal thrusts if back slaps are ineffective. For unconscious adults and children, chest thrusts are suggested. Stay updated with these life-saving techniques and recommendations by certifying or recertifying in Basic Life Support.
COVID-19 in Basic Life Support and First Aid
 Since the COVID-19 pandemic, the ILCOR has released potential impacts of the virus on resuscitation. Despite the contagious nature of the pandemic, the ILCOR continues to suggest lay rescuers perform CPR when possible and use appropriate PPE to protect themselves from the virus.
Since the COVID-19 pandemic, the ILCOR has released potential impacts of the virus on resuscitation. Despite the contagious nature of the pandemic, the ILCOR continues to suggest lay rescuers perform CPR when possible and use appropriate PPE to protect themselves from the virus.
We have since designed algorithms specific to treating either suspected or confirmed patients of COVID-19 so that rescuers can still perform life-saving actions on these individuals without disregarding their expected state. As the ILCOR continues to release its findings and conclusions on more long-term COVID-19 studies, we will continue to update our content accordingly.
What’s Coming Next?
Medical content is constantly evolving and updating. As the ILCOR continues to release its recommendations, we will continue to review its research and update our content accordingly. It is important to stay up-to-date with the most current guidelines, and at Save a Life, we are committed to keeping our life-saving information accurate.
Be sure to check back in on our Journal Articles regularly for further updates. Until then, enroll in one of our courses today to ensure you are receiving the most recent life-saving information! Share your experience of learning in the comments section below or in our online community.









Leave a Reply