Your cart is currently empty!
How to Stay Atop and Follow the ACLS Algorithms
Completing a life-saving review of the ACLS algorithm is the best way to reduce the mortality risk among those under your care when cardiac arrest or a cardiovascular health care emergency, including stroke, strikes. According to the International Liaison Committee on Resuscitation (ILCOR), more than 350,000 Americans suffer out-of-hospital arrest annually, as well as 209,000 people that suffer cardiac arrest in the hospital. Yet, as few as 12 percent survive, depending on where the arrest occurred. These statistics reveal the importance of staying atop the algorithm and its best practices.
Since each minute between entering arrest and the initiation of CPR and ACLS increases risk of poor outcomes, staying atop ACLS standards will help you save lives. Unfortunately, the stress associated with working in health care facilities can make staying updated difficult at best, so health care providers should complete a review of the algorithm often and follow a few best practices to commit it to memory.
Key Highlights of the ACLS Algorithm for Cardiac Issues
The ACLS algorithm includes detailed recommendations for the treatment of acute coronary syndrome, bradycardia with a pulse, and tachycardia with a pulse. The algorithms vary slightly but all advise common actions, including:
1. Completion of the ABCD’s of ACLS, as well as preparation for potential cardiac arrest. The ABCD’s refer to:
- Airway – The airway may become occluded due to a foreign object lodged in the throat or another adverse event, such as a severe allergic reaction. If an airway cannot be established quickly, health care providers should consider establishing an advanced airway as necessary within the algorithm.
- Breathing – Regardless of known health conditions, patients suffering from a cardiovascular emergency requiring ACLS should be given 100-percent oxygen, but it is important to avoid over-ventilation. Over-ventilation may lead to tissue damage and even ketoacidosis from a buildup of carbon dioxide molecules in the bloodstream.
- Circulation – Poor circulation in the body results in hypoxia and may lead to severe patient outcomes, and this is why high-quality chest compressions are essential in performing CPR and ACLS. The chest compression rate is standardized at 100 compressions per minute for all individuals, and while checking for a pulse is still required, health care providers must not mistake the residual beat of chest compressions as an actual heartbeat. Therefore, failure to identify a pulse within five seconds should result in the continuation of chest compressions and the subsequent steps in the algorithm.
- Differential diagnosis – Differential diagnosis is often mistaken for defibrillation in the algorithm, but since fibrillation often results from a given cause of arrest, the Hs and Ts, determining a cause of arrest takes priority. Obviously, defibrillation will be necessary for a patient suffering from a shockable rhythm, but the only way to truly treat cardiac arrest in this circumstance hinges on reversing its cause.
2. Administration of morphine, nitroglycerin, oxygen and aspirin as necessary.
3. Obtaining a 12-lead EKG.
4. Proceeding with adjunctive therapies for ST elevation or admission to the emergency department with a series of lab work, including drawing a troponin level, continuous monitoring of heart rhythms.
5. Depending on the severity of the condition, administration of other treatments and consultation with cardiology for cardiac catheterization may be necessary.
A Two-Minute Review of ACLS for Stroke
Stroke takes the lives of 140,000 Americans annually, and someone suffers a stroke every 40 seconds. The majority of strokes result from blockage of blood flow to the brain and cost more than $34 billion per year, asserts CDC.gov. Left untreated, stroke may result in serious physical injury, loss of cognitive function and even death, but the ACLS protocols within the algorithm provide a series of steps to reduce poor outcomes. The steps are as follows:
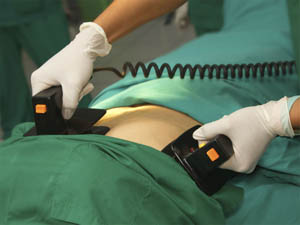 EMTs should complete a prehospital stroke assessment, document time of occurrence and symptoms severity, check glucose levels and alert hospital staff before arrival.
EMTs should complete a prehospital stroke assessment, document time of occurrence and symptoms severity, check glucose levels and alert hospital staff before arrival.- Upon arrival, the algorithm recommends a comprehensive assessment of vital signs, heart function, treatment of hypoxia and extreme glucose levels (if necessary), ordering an MRI of the brain and activation of the stroke team.
- The stroke team should complete a neurologic examination and review patient history and symptoms.
- Depending on the results of advanced imaging, fibrinolytic therapy or admission to an ICU or stroke unit may be appropriate.
What About Review of Advanced Care for the Choking Victim
The algorithm does not necessarily define the practices for caring for those suffering from choking. However, the best practices for treating the unconscious choking victim mirror the standard ACLS and CPR algorithm. Chest compressions should dislodge the object, but if unsuccessful, the person will likely enter cardiac arrest within minutes.
When attempting to administer rescue breaths to someone suspected of choking, air may not go in. In this situation, perform the head-tilt, chin-lift maneuver, provided the object is not visible in the person’s mouth. If the object is visible and dislodged, attempt to remove it with a finger-sweep. Continue with chest compressions in rounds of 30, checking for the object between intervals. At the same time, attempt to administer rescue breaths.
Most importantly, do not attempt to remove an object that does not appear to be dislodged or easily removed with a finger sweep. This may push the object further into the throat, exacerbating the problem.
Health care providers that have never been in this predicament before may be concerned about the need to check for a pulse. It’s a near-waste of time as the chest compressions in an attempt to dislodge the object will provide circulation in the interim. However, the ACLS algorithm does recommend the use of an EKG to assess rhythm and the establishment of an advanced airway after four minutes of performing chest compressions or after two minutes if the person enters a non-shockable rhythm.
It is reasonable to assume someone that loses consciousness has likely entered an arrhythmia, so the primary ACLS protocol takes precedence, excluding the need to check for the object in the mouth.
Ultimately, the unconscious choking victim will need CPR and ACLS in order to survive, especially if the object cannot be dislodged in a reasonably short time after losing consciousness.
Even in circumstances where the object is dislodged, breathing resumes, and ROSC is achieved, aspiration may have occurred. Unfortunately, aspiration may contribute to the recurrence of cardiac arrest and pulmonary problems, including pneumonia. Therefore, health care professionals should proceed with the facility-specific protocols for obtaining a chest X-ray and treating possible cases of aspiration.
The Overarching Algorithm
ACLS gives health care providers a means of treating individuals in a way that increases their chances of survival. The differences in the algorithm vary slightly by suspected cause, as noted above. At the same time, the dominant algorithm, asserts ECCGuidelines.Heart.Org, remains the same.
The algorithm advises:
- Start CPR. The initiation of CPR includes attaching the monitor or defibrillator and administering oxygen. However, this may not be possible for out-of-hospital arrest. In such cases, standard CPR procedures may be initiated. If all else fails, hands-only CPR is the best way to go.
- Determine whether the rhythm’s shockable or not. Shockable rhythms, such as ventricular fibrillation (VF) or polymorphous ventricular tachycardia (pVT), should be treated with a shock. Non-shockable rhythms include pulseless electrical activity (PEA) and asystole.
- Regardless of whether a shock was administered, the next step is identical, comprised of performing CPR for two minutes, and establishing an intravenous (IV) or intraosseous (IO) access. Those suffering from a non-shockable rhythm should be given epinephrine at this point. Those with shockable rhythms may receive another shock, but afterward, continue CPR for two minutes and administer epinephrine.
- The key difference is simple: non-shockable gets epinephrine after two minutes of determining rhythm; shockable gets epinephrine after four minutes.
- If the person continues with a shockable rhythm, without return of spontaneous circulation (ROSC), continue CPR for two minutes and administer amiodarone. At this point, treat the reversible causes of arrest.
- Someone without a shockable rhythm after completing the first two minutes of CPR after determining a non-shockable rhythm and administering epinephrine should receive an additional two minutes of CPR. Next, health care professionals must treat reversible causes.
- A final key difference between the overarching algorithm is the administration of amiodarone. Amiodarone is only administered for those in a shockable rhythm. It should not be administered for those in a non-shockable rhythm.
Top Four Tips to Remember ACLS
Health care professionals should follow these tips to commit the variances and similarities of the algorithms to memory.
- Enroll in an online review and training course. An online review course is an excellent way to help busy health care professionals stay up-to-date on the details of ACLS. In addition, research suggests, reports the National Library of Medicine, little difference in efficacy among health care students, including nursing students, that have completed an online versus in-person course. In other words, completing an online course is just as effective as completing an in-person course. That being said, individual facilities may require additional, in-person training sessions for employment, and such facilities have discretion to adjust the algorithms to meet the unique needs of the population served. For instance, those working in areas where drowning or exposure to the elements are more likely to occur may have additional ACLS requirements and training sessions to complete, beyond the typical training available online. To ensure uninterrupted employment, make sure your credentials are up-to-date and reflect the standards of both the ILCOR and your specific facility.
- Participate in online simulation training scenarios for ACLS, like Megacodes. Megacodes training scenarios are short, online sessions that provide users with a hypothetical patient and problem. The user must identify the cause and answer questions based on symptoms and assessment within three to five minutes, reflecting the time that passes when running a code.
- Review the ILCOR for updated ACLS recommendations. While the ILCOR publishes broad updates to the algorithm every five years, new research and information may lead to changes in recommendations during any year. The ILCOR recognizes the ongoing need to use the latest best practices to improve treatment outcomes, but the responsibility of knowing these changes falls to the health care provider. In addition, the timeline between certification and expiration, if applicable, means health care providers that completed a course last year, or even six months prior, may not have seen the latest recommendations. This is why reviewing the materials online regularly to check for new updates is essential.
- Hold and participate in mock code drills in your organization. Mock code drills are similar to the Megacodes training scenarios, but these take place within your facility. They may involve a mannequin or other equipment to ensure everyone understands their roles in providing the right care to someone suffering from a cardiovascular emergency. Mock code drills may be held for suspected stroke, sudden cardiac arrest, and heart attack. Depending on your facility, these drills may be conducted with a frequency that is suitable for the type of care setting. For example, health care professionals working in ICU may be required to participate in mock drills more often than staff members working in Medical-Surgical units. The difference in frequency effectively provides extra opportunities for staff members to refine and review their ACLS skills when working in care settings where arrest is more likely to occur.
Know When to Renew Your ACLS Certification and Its Fundamentals
Mortality from cardiac arrest and poor treatment outcomes from both cardiac arrest and medical emergencies can be successfully reduced through the application of CPR and the ACLS Algorithm. While the algorithm is typically associated with cardiac arrest, it’s also applicable to stroke and arrhythmias or heart problems, such as a heart attack, which may precede cardiac arrest. Thus, it is essential to review your ACLS skills often and ensure their accuracy.
Do you have any tried and true methods for remembering the ACLS skills and its algorithms? Share them along with this article to social media now. Also, recognize the importance of staying up to date on the algorithm, and remember to enroll in your advanced life-saving skills course today. By staying atop the latest information, you can save more lives.









Leave a Reply