Your cart is currently empty!
Top 9 Fundamentals of Online Bloodborne Pathogens
Bloodborne illnesses have a dark, sordid history. They have led to major health outbreaks and traumatic loss of life, but history teaches a vital lesson about controlling the spread of these diseases. As the name suggests, bloodborne illnesses spread through blood and other potentially infectious materials (OPIM), and health care workers may encounter such pathogens as part of their job duties.
Therefore, the Occupational Safety and Health Administration (OSHA) requires health care facilities, as well as any other employer where workers may come into contact with such substances, to maintain strict compliance with regulations.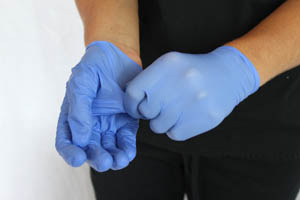 These regulations include creating an exposure control plan, completing OSHA-mandated training, such as an online Bloodborne Pathogens (BBP) course, and more.
These regulations include creating an exposure control plan, completing OSHA-mandated training, such as an online Bloodborne Pathogens (BBP) course, and more.
The best way to prevent the spread of BBP in the workplace is to understand more about the most common BBP, how they may be transmitted in the course of work, how to clean up after providing care, and what to do if an exposure incident occurs. Completing BBP training effectively helps you protect yourself and those around you from BBP. Consider these 10 fundamentals of BBP courses and their usefulness in reducing the spread of illness.
1. An Online BBP Course Provides an Education of the Most Common Pathogens
Health care workers may encounter blood or potentially infectious bodily fluids in many ways. According to the Centers for Disease Control and Prevention (CDC), the most common BBP in health care include the human immunodeficiency virus (HIV) and the Hepatitis B and Hepatitis C viruses (HBV and HCV). Although thousands of potentially harmful pathogens exist, these three represent the greatest risk to health care workers. They may spread through blood and bodily fluids that may contain blood.
According to CDC.gov, the agency received 3,218 reports of HBV in 2016, but due to under-reporting and inaccurate diagnoses, actual case statistics may have exceeded 20,000. Meanwhile, similar rates were reported to the CDC for HCV, but the rate of under-reporting pushes the actual prevalence to more than 41,000.
Among these three BBP, the prevalence of HIV, notes the CDC, is even higher at 1.1 million people over age 13 living with the illness in the U.S. Although rates have declined for decades, the risk remains, and health care professionals need to know that there is a strong likelihood they will care for someone with one of these three illnesses.
2. Students Learn More About OSHA’s Standards
The OSHA Standard for BBP requires employers take a proactive approach to prevent the spread of BBP.
This includes the following:
-
- Create an exposure control plan.
- Update the plan annually to reflect recent changes in risk or new bloodborne diseases that have risen in prevalence.
- Follow universal precautions.
- Use engineering controls to reduce risk.
- Use work practice controls to ensure proper handling of infectious materials.
- Provide personal protective equipment.
- Make HBV vaccines available to all workers.
- Establish post-exposure evaluation and follow-up protocols.
- Use labels to communicate hazards.
- Provide training to workers.
- Maintain worker medical and training records.
3. Participants Gain an Understanding of How BBP Transmission Occurs
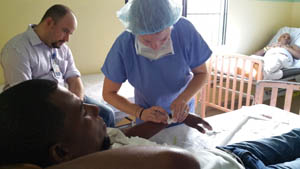 In the discussion of BBP, the risk of exposure to a bloodborne illness can be confusing. The risk lies in potential transmission of the pathogen from one person to another. Bloodborne illnesses are the result of direct contact between an infectious agent and the mucous membranes of another person. Mucous membranes are any surface where the skin ends. Such surfaces allow a pathogen to enter the body.
In the discussion of BBP, the risk of exposure to a bloodborne illness can be confusing. The risk lies in potential transmission of the pathogen from one person to another. Bloodborne illnesses are the result of direct contact between an infectious agent and the mucous membranes of another person. Mucous membranes are any surface where the skin ends. Such surfaces allow a pathogen to enter the body.
For example, the eyes, open wounds, nose, and mouth are mucous membranes. Anything contaminated with blood or OPIM, such as dirty glove or garment, that subsequently touches a mucous membrane results in transmission. Additional examples of how transmission occurs include splashes, providing care to someone bleeding profusely, disposal of feces or urine, or even sharps’ injuries, such as a needlestick.
It also pertinent to reiterate the need to follow universal precautions, treating any fluid as containing the deadliest pathogen in the world.
4. Objectives Teach What Constitutes Exposure and Exposure Incidents
Exposure to a pathogen does not refer to transmission. Instead, it focuses on the actions during which a person may encounter bloodborne viruses or bacteria. This may include helping with activities of daily living, administering injected medications, checking blood-glucose levels, cleaning up messes, and more.
On the other hand, an exposure incident occurs when an employee that is working encounters blood or OPIM in a manner that is consistent with transmission. In other words, accidentally splashing blood or OPIM into the face and needlesticks are types of exposure incidents.
5. It Includes a Review of General Exposure Control Plans
The exposure control plan is a written protocol for employees to reduce their risk of exposure incidents bloodborne illnesses. A typical exposure plan will list all job classifications in which workers may encounter such pathogens, and it will help those new to the field understand what activities may result in exposure. An exposure plan ensures all workers understand the risk of transmission and subsequent illnesses associated with such exposure.
The plan may seem counterproductive and discouraging to workers entering a new field, such as ancillary positions in health care. However, the exposure control plan enhances everyone’s safety by ensuring all team members work together to prevent infection. In a sense, the plan announces the potential risk and why it exists. Therefore, workers can take appropriate actions to prepare for such exposure, such as completing an online Bloodborne Pathogens training course.
The plan also includes a full breakdown of what to expect after an exposure incident, including:
-
-
- Immediately report an exposure incident to your supervisor. Depending on the pathogen in question, it may be possible to reduce the chances of full incubation and subsequent infection. However, interventions must begin within hours, not days.
- Exposure results will take time. After exposure, a full series of labs will determine any pre-existing conditions that were undiagnosed prior to the incident. Results of possible infections can take days to ascertain, and retesting will be necessary.
- Employers will need to complete OSHA FORM 300. According to OSHA.gov, the completion of this form is necessary to document and track workplace injuries and subsequent ailments resulting from an exposure incident.
- Facility-specific guidelines will determine who pays for treatment. Only the employer can provide information regarding financial responsibility for testing and treatment following an incident. You may also need to submit medical documentation for tracking and monitoring purposes.
-
6. Training Ensures Proper Donning, Use and Removal of Personal Protective Equipment
 Personal protective equipment describes the protective clothing, goggles, face shields, gloves and other equipment used to prevent an exposure incident. However, this equipment may incur damage in the course of work, which may result in an exposure incident.
Personal protective equipment describes the protective clothing, goggles, face shields, gloves and other equipment used to prevent an exposure incident. However, this equipment may incur damage in the course of work, which may result in an exposure incident.
Preventing an incident also necessitates an understanding of how properly apply, use, and remove personal protective equipment. Secure all ties and straps. Take care to avoid undue damage to such equipment. When removing personal protective equipment, avoid making unnecessary contact with surfaces exposed to BBP.
Remove equipment slowly, minimizing the accidental spread of contaminated materials. When removing gloves, pull on the center of the glove slightly with the opposing hand. This will cause the wrist portion to roll. Continue pulling on the glove until it slips off the hand, rolling the used glove into a ball with the hand that remains protected. Using the non-gloved fingers, slide fingers up under the remaining glove to roll the wrist opening upward. Touching on the inside of the glove, pull the glove upward into an inside-out ball. Dispose of gloves in an appropriate container.
7. Individuals Enrolled in the Course Learn How to Address the Mess
Students that complete an appropriate course also learn how to thoroughly clean up blood and contaminated materials. Depending on the substance, contamination protocols may include using solidifier and an approved disinfectant. All contaminated, disposable items should be placed in red, biohazard bags and into appropriate, biohazard containers. Used sharps should be disposed of in a labeled, red sharps container. Similar protocols exist for cleaning of contaminated linens and clothing, placing into a proper bag and sent for appropriate cleaning. However, such protocols will depend on your facility. One more thing, it is against regulations to recap sharps, and most sharps have a built-in closure device. For instance, syringes may have a built-in lock that covers the needle, but any recapping with the removable cap will incur a fine during an inspection.
8. Students Learn Where and When Exposure May Occur
Another aspect of the course goes back to where and when exposure to may occur. Although exposure activities can be common, the places of exposure are much more common than you may realize.
For example, non-health care workers, including daycare providers, teachers, coaches, security guards, officers, tattoo artists, property managers, social workers, occupational and physical therapists, sanitation workers, and custodians, may encounter BBP.
9. Participants Also Revisit the Omnipotent Role of Handwashing
Any education on BBP must include a comprehensive review of proper hand washing protocols. This includes using warm water, ensuring access to clean, non-contaminated towels, scrubbing all surfaces of the hands and two inches up the wrist for at least 20 seconds, and rinsing with the fingers pointed down, preventing pathogen-rich water from running up the arm. Dry with a clean towel, but it is easy to overlook a few final steps after rinsing the hands.
Throw the used, disposable towel into the trash immediately. Never use a wet towel for to shut off water or open doors. Even a small amount of water in a towel can enable pathogens to spread from surfaces to your hands. Use a clean towel to shut off the water, dispose of it, and use another clean towel to open the door, if necessary.
More than anything else, remember hand washing is the most crucial step in preventing the spread of all pathogens. Failure to wash your hands regularly could lead to unexpected illness. Any instance where contact with other people or objects may occur should follow with hand washing, and always wash your hands before eating or drinking.
Know the Fundamentals of an Online Bloodborne Pathogens Course
The risk of exposure will always exist in varying fields. Even if vaccines do become available for major BBP, including HIV, the risk for contracting an illness from someone due to an exposure incident will remain. The first step to reducing the spread of any illness begins with knowing more about its mode of transmission, and the design of an online Bloodborne Pathogens training course provides this knowledge. Protect yourself with the information to handle blood and OPIM properly in all of life’s situations. Since the most common bloodborne illnesses can and do contribute to a higher risk of death, completing an online Bloodborne Pathogens course could save your life.
Do you have any thoughts on how health care providers can work to reduce the spread of bloodborne pathogens? Share this article and your views on social media now. Also, remember to enroll in your OSHA-mandated course today.









Leave a Reply