Your cart is currently empty!
Tachycardia is defined as a heart rate greater than what is considered normal for a child’s age. Like bradycardia, tachycardia can be life-threatening if it compromises the heart’s ability to perfuse effectively. When the heart beats too quickly, there is a shortened relaxation phase. This causes two main problems: the ventricles are unable to fill completely, so cardiac output is lowered; and the coronary arteries receive less blood, so supply to the heart is decreased.
There are several kinds of tachycardia, and they can be difficult to differentiate in children on ECG due to the elevated heart rate.
Pediatric tachyarrhythmias are first divided into narrow complex or wide complex tachycardia. Measure the QRS complex on a standard ECG to assess its width.
| NARROW QRS COMPLEX (≤ 0.09 S) | WIDE QRS COMPLEX (> 0.09 S) |
|---|---|
| Atrial fibrillation or Atrial flutter | Ventricular tachycardia |
| Sinus tachycardia | Unusual SVT |
| Supraventricular Tachycardia (SVT) |
Atrial flutter is an uncommon rhythm distinguished on an ECG as a sawtooth pattern. It is caused by an abnormal pathway that causes the atria to beat very quickly and ineffectively. Atrial contractions may exceed 300 bpm but not all of these will reach the AV node and cause a ventricular contraction.
Most often, PALS providers will have to distinguish between two similar narrow QRS complex tachyarrhythmias: sinus tachycardia and supraventricular tachycardia (SVT). SVT is more commonly caused by accessory pathway reentry, AV node reentry, and ectopic atrial focus.
| SINUS TACHYCARDIA | SUPRAVENTRICULAR TACHYCARDIA |
|---|---|
| Infant: < 220 bpm | Infant: > 220 bpm |
| Child: < 180 bpm | Child: > 180 bpm |
| Slow onset | Abrupt start/stop |
| Fever, hypovolemia | Pulmonary edema |
| Varies with stimulation | Constant, fast rate |
| Visible P waves | Absent P waves |
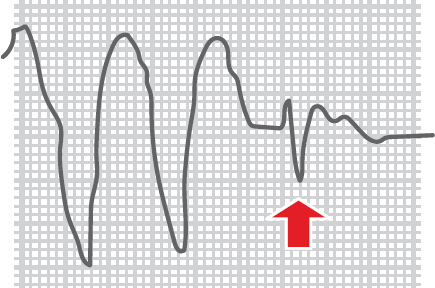
Ventricular tachycardia (VT) is uncommon in children but can be rapidly fatal. Unless the person has a documented wide complex tachyarrhythmia, an ECG with a QRS complex greater than 0.09 seconds is VT until proven otherwise. Polymorphic VT, Torsades de Pointes, and unusual SVT (SVT with wide complexes due to aberrant conduction) may be reversible, e.g. magnesium for Torsades, but do not delay treatment for VT. Any of these rhythms can devolve into ventricular fibrillation (VF). VT may not be particularly rapid (simply greater than 120 bpm) but is regular. Generally, P waves are lost during VT or become dissociated from the QRS complex. Fusion beats are a sign of VT and are produced when both a supraventricular and ventricular impulse combine to produce a hybrid appearing QRS (fusion beat) (Figure 14).