Your cart is currently empty!
Monitor and maintain an open airway at all times. The provider must decide if the benefit of adding an advanced airway outweighs the risk of pausing CPR. If the individual’s chest is rising without using an advanced airway, continue giving CPR without pausing. However, if you are in a hospital or near trained professionals who can efficiently insert and use the airway, consider pausing CPR.
In cardiac arrest, administer 100% oxygen. Keep blood O2 saturation (sats) greater than or equal to 94 percent as measured by a pulse oximeter. Use quantitative waveform capnography when possible. The normal partial pressure of CO2 is between 35 to 40 mmHg. High-quality CPR should produce a ETCO2 between 10 to 20 mmHg. If the ETCO2 reading is less than 10 mmHg after 20 minutes of CPR for an intubated individual, then you may consider stopping resuscitation attempts.
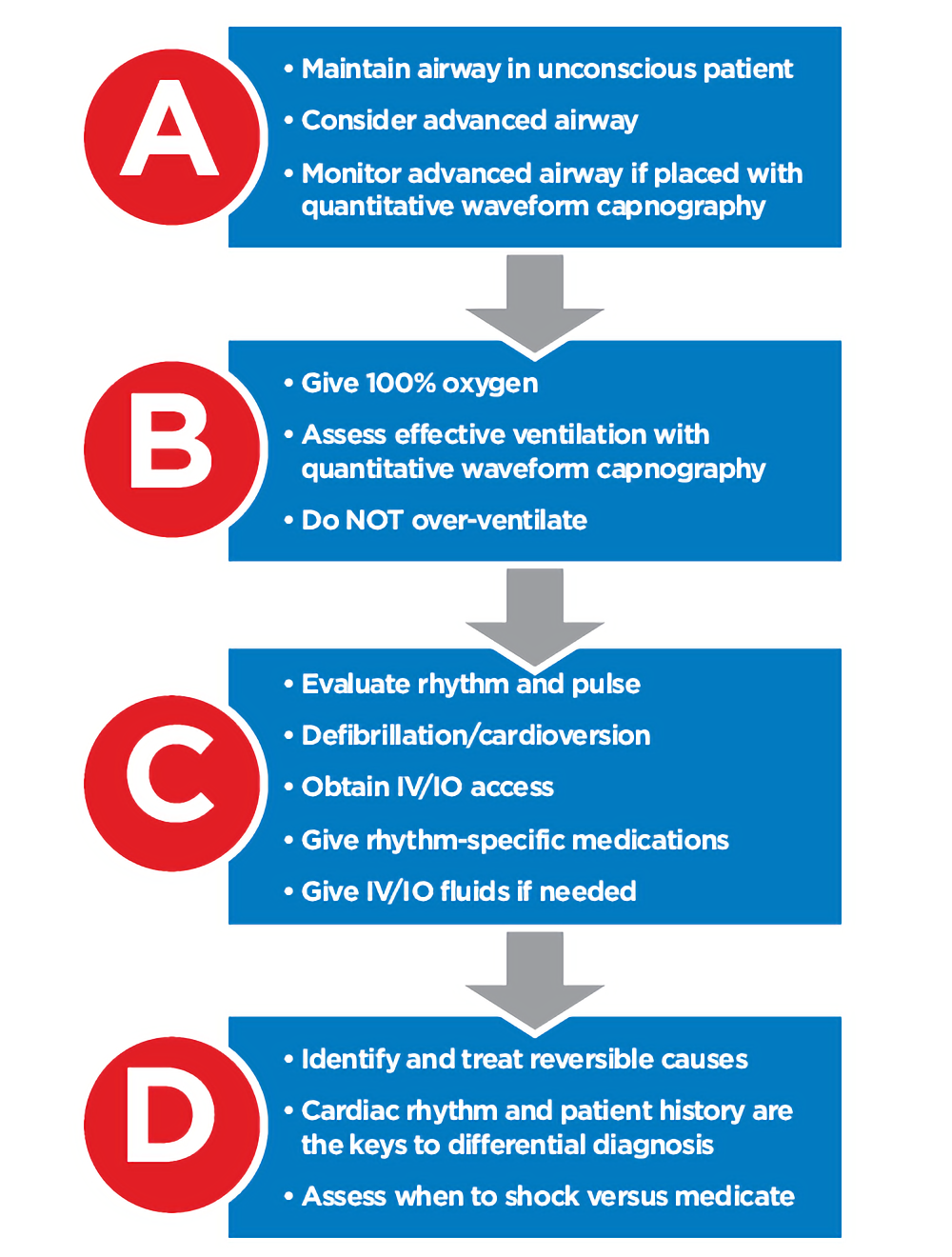
Obtain intravenous (IV) access when possible. However, if after two unsuccessful attempts, go straight to intraosseous access (IO). Monitor blood pressure with a blood pressure cuff or intra-arterial line if available. Monitor the heart rhythm using pads and a cardiac monitor. When using an AED, follow the directions (i.e., shock a shockable rhythm). Give fluids when appropriate. Use cardiovascular medications when indicated.
Start with the most likely cause of the arrest and then assess for less likely causes. Treat reversible causes and continue CPR as you create a differential diagnosis. Stop only briefly to confirm a diagnosis or to treat reversible causes. Minimizing interruptions in perfusion is key.